Yes, eyelashes can and usually do grow back after blepharitis, but how fully and how fast depends almost entirely on whether the inflammation has damaged your follicles. If the follicles are intact, expect to see noticeable regrowth in roughly 6 to 12 weeks. If blepharitis has been chronic, severe, or repeatedly ulcerative, there is a real risk of scarring at the eyelid margin that can make some lash loss permanent. The sooner you get the inflammation under control, the better your odds of a full recovery.
Do Eyelashes Grow Back After Blepharitis? Timeline and Tips
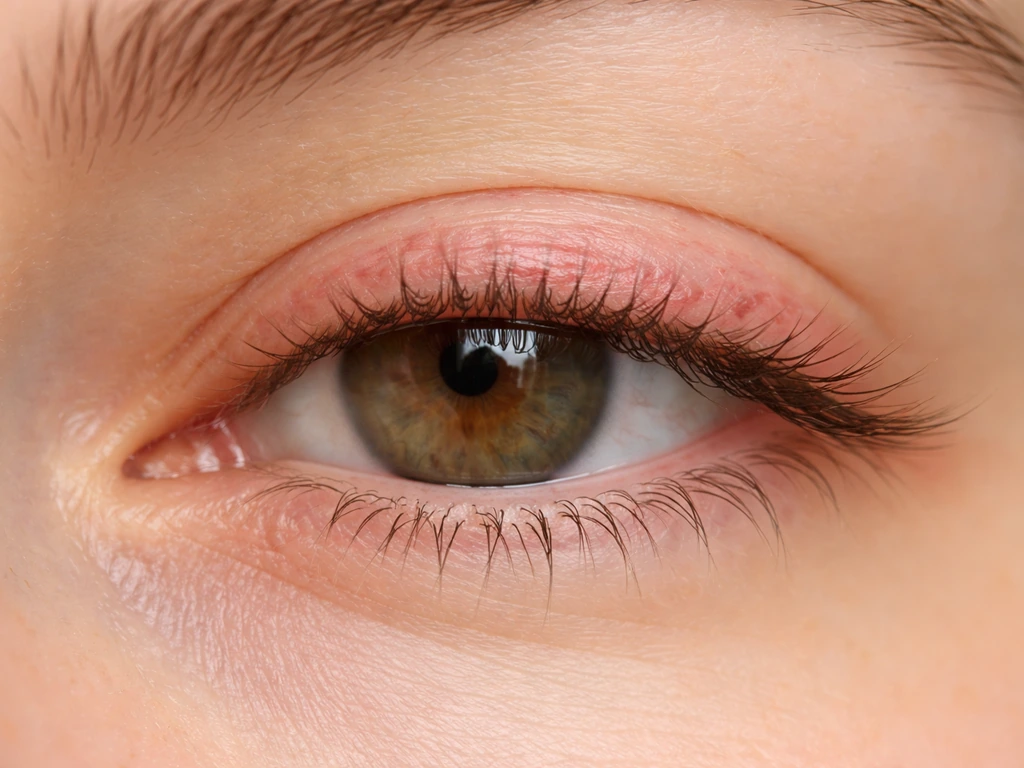
How eyelash growth works (and why they fall out in the first place)

Each eyelash follows a three-stage cycle: anagen (active growth), catagen (transition), and telogen (resting), before the lash sheds and the whole process starts over. The catagen phase alone lasts around 15 days, and the full cycle from growth to shed is much shorter than scalp hair, which is why lashes stay short. Once a lash sheds naturally, the follicle rests, then re-enters anagen and produces a new lash. The whole trip from bare follicle to visible lash takes roughly 6 weeks under ideal conditions, and full length can take closer to 12 weeks.
Lashes fall out faster than normal when something disrupts this cycle. Eyelid inflammation is one of the most common culprits because the follicle sits right at the eyelid margin, exactly where blepharitis does its damage. Rubbing, scaling, and bacterial activity at the follicle opening can push lashes prematurely into telogen, causing shedding that looks alarming but is often reversible. The critical variable is whether the follicle itself survives the inflammation intact.
What blepharitis actually does to your lash follicles
Blepharitis comes in two main forms: anterior blepharitis, which affects the front of the eyelid where the lashes emerge, and posterior blepharitis, which targets the meibomian glands further back on the lid margin. Anterior blepharitis hits lash follicles directly. Bacteria (commonly Staphylococcus) infect the base of the lashes, causing crusting, inflammation, and in ulcerative cases, small ulcers right at the follicle openings. Posterior blepharitis, often tied to meibomian gland dysfunction, causes poor tear film quality and chronic lid-margin irritation that creates a hostile environment for lash cycling even when it doesn't directly attack follicles.
The specific complication to understand here is called madarosis, which is the medical term for eyelash loss associated with blepharitis. Another is trichiasis, where lashes grow back but in the wrong direction, pointing toward the eye instead of away. Both appear in clinical descriptions of blepharitis as recognized complications, not rare edge cases. Trichiasis itself is a sign of significant eyelid margin disease and sometimes needs procedural treatment. Demodex mite infestation, a cause of chronic blepharitis, is particularly linked to persistent inflammation that grinds down the lid margin over time.
The worst-case scenario is scarring. Recurrent ulcerative blepharitis can leave scar tissue at the eyelid margin. When inflammation destroys a follicle and fibrosis replaces it, that follicle cannot regenerate. This is the same final pathway as cicatricial (scarring) alopecia on the scalp: inflammation destroys the follicular unit, fibrous tissue fills the space, and regrowth becomes impossible in that specific spot. Histological confirmation is the most reliable way to distinguish scarring from non-scarring loss, which is why a proper clinical evaluation matters when loss is severe or prolonged.
Do eyelashes grow back? Timelines and what affects the speed

For most people with mild to moderate blepharitis who treat it promptly, yes, lashes grow back. If you are wondering about later-life timelines, see Do eyelashes grow back after 50 for how age can change recovery expectations. The practical timeline once inflammation is controlled is 6 to 12 weeks for visible regrowth, with the lash line looking fuller closer to the 3-month mark. That said, several factors push the timeline in either direction.
| Factor | Effect on Regrowth Timeline |
|---|---|
| Mild, acute blepharitis treated quickly | Regrowth likely within 6–12 weeks |
| Chronic untreated blepharitis | Delayed; ongoing inflammation keeps disrupting the cycle |
| Ulcerative blepharitis with scarring | Partial or no regrowth in scarred areas |
| Demodex infestation (active) | Slow or incomplete until mites are eliminated |
| Age (over 50) | Anagen phase shortens naturally, slowing recovery |
| Meibomian gland dysfunction alongside blepharitis | Poor lid-margin environment slows follicle recovery |
| Post-inflammatory but intact follicles | Normal cycle resumes; full regrowth expected |
The biggest factor is whether treatment is in place. Blepharitis is a condition that rarely cures itself permanently but responds well to consistent management. Until the inflammation is addressed, the follicle environment stays disrupted and regrowth stalls. Think of it like trying to grow grass while someone keeps pouring salt on the soil.
People dealing with other causes of lash disruption, like hormonal changes after pregnancy or menopause, or lash loss following chemotherapy, often find the timeline question similar but the mechanism different. If you notice lash shedding after pregnancy, it can also be tied to hormone shifts and may improve as your eyelid health and hormone levels stabilize hormonal changes after pregnancy. If you lost lashes after chemotherapy, the timeline can still be similar, but regrowth depends on whether the follicle was damaged and whether there is any ongoing eyelid inflammation. With blepharitis the driver is active inflammation at the follicle site, so managing that inflammation is the central lever.
Regrowth after eyelid surgery (blepharoplasty): what's normal and what isn't
If you've had blepharoplasty (eyelid surgery) and you're now dealing with lash changes, the situation is a little different but the core biology still applies. Research looking at full-thickness eyelid resections found that surgical removal of eyelid margin tissue typically does not significantly reduce postoperative lash numbers, which suggests follicles show more resilience to surgical trauma than you might expect. That's actually reassuring if you're worried that the procedure itself wiped out your lash line.
What does happen after blepharoplasty is that the local environment around the eyelid gets temporarily disrupted. Tear film parameters, for example, show measurable changes after upper eyelid blepharoplasty, though studies show these generally return to baseline by around 6 months. An irritated, inflamed post-surgical eyelid is not an ideal environment for lash cycling, so some temporary thinning or shedding in the weeks after surgery is not unusual. Post-op instructions typically ask you to avoid makeup around incisions for at least the first 7 days, partly to reduce chemical and mechanical irritation that could worsen inflammation near the follicles.
What should prompt a call to your surgeon: lash loss that progresses beyond 3 months post-op without stabilizing, noticeable scarring at the lash line, misdirected lashes rubbing the cornea, or any sign of persistent eyelid margin infection. A normal post-blepharoplasty recovery involves gradual improvement, not worsening lash density over time.
What to do right now: treating blepharitis and protecting your follicles

The most important thing you can do today is start a consistent lid hygiene routine. Cochrane evidence shows that lid hygiene provides symptomatic relief in both anterior and posterior blepharitis, even though no treatment fully cures it permanently. It won't reverse follicle damage that's already done, but it stops further damage and creates the conditions for regrowth.
- Warm compress: Apply a warm (not hot) compress to closed eyelids for 5 to 10 minutes. This softens debris at the lash base and helps unblock meibomian glands in posterior blepharitis.
- Lid massage: After the compress, gently massage along the eyelid margin to encourage gland drainage.
- Lid scrub: Using a clean cotton pad or washcloth with diluted baby shampoo or a purpose-made eyelid cleanser, gently scrub the base of the lashes to remove crusts and bacterial/mite debris. Research-backed options include terpinen-4-ol based scrubs (like Cliradex) for Demodex blepharitis.
- Frequency: Do this once or twice daily during active flare-ups, then daily or every other day for maintenance.
- Avoid eye makeup during active inflammation: Mascara and eyeliner applied to an inflamed lid margin can introduce more bacteria, clog follicle openings, and mechanically stress already-fragile lashes.
- Stop rubbing your eyes: It seems obvious but chronic rubbing physically accelerates lash shedding and traumatizes the lid margin.
For Demodex blepharitis specifically, standard lid hygiene has limits. FDA-approved lotilaner ophthalmic solution (Xdemvy) was validated in trials of 833 patients and is the first targeted prescription treatment for Demodex blepharitis. If your blepharitis has been diagnosed as Demodex-related and basic hygiene isn't moving the needle, this is worth discussing with your eye doctor. Reducing the mite burden directly reduces the chronic inflammatory signal that keeps follicles suppressed.
Supporting regrowth: serums, castor oil, biotin, and what the evidence actually says
Once inflammation is under control, there are a handful of evidence-graded options for supporting lash regrowth. Here's an honest look at each.
Prescription lash serums (bimatoprost)
Bimatoprost ophthalmic solution 0.03% is FDA-approved for eyelash hypotrichosis (sparse lashes) and works by extending the anagen (growth) phase. Clinical prescribing data confirms it increases lash length, thickness, and darkness. It is the most evidence-backed option available. The catch: it requires a prescription, and lash enhancement reverses after discontinuation, returning to pre-treatment levels. It also carries real side effects including eye irritation, conjunctival redness, and possible skin pigmentation around the eye. It should be used with caution if you have active ocular inflammation, which is important context when you're managing blepharitis simultaneously. Discuss timing with your eye doctor before starting.
Castor oil
Castor oil is probably the most popular natural remedy for lash growth, but the evidence picture is mixed. There is no clinical research specifically on castor oil for eyelash growth in the way supplement or cosmetic marketing presents it. However, a randomized trial on topical periocular castor oil for blepharitis found clinical improvements in eyelid margin thickening, lash matting, madarosis, and other blepharitis markers compared to control. So castor oil's relevance to lash recovery in blepharitis may be more about managing the inflammatory condition itself than directly stimulating follicles. Applied carefully along the lash line at night with a clean brush or cotton swab, it's low-risk. Just don't expect magic and don't apply it during active, weeping inflammation.
Biotin
Biotin supplements are heavily marketed for hair and lash growth, but a recent systematic review concluded that current evidence does not support routine biotin supplementation for alopecia-related hair loss in people without a documented deficiency. Biotin deficiency is real and does cause hair and lash thinning (along with symptoms like conjunctivitis and skin rash), so supplementing helps if you're actually deficient. If you're not deficient, adding more biotin to your diet likely does nothing for your lash line. A standard diet with eggs, nuts, and legumes usually covers your biotin needs. It's not harmful to supplement, but don't invest your expectations in it as a standalone regrowth solution.
What to avoid
- Eyelash extensions while blepharitis is active: adhesives and mechanical weight stress already-fragile follicles and can make the inflammatory cycle worse.
- Waterproof mascara during recovery: harder to remove without heavy rubbing, which traumatizes the lash line.
- Sharing eye makeup or applicators: high bacterial transmission risk when your eyelid barrier is already compromised.
- Aggressive rubbing to remove eye makeup: use a gentle, oil-based remover and press rather than drag.
- Unverified lash growth products with irritating ingredients: fragrances, alcohols, and certain preservatives can aggravate an already-inflamed eyelid margin.
When to see an eye doctor

Blepharitis usually does not cause permanent damage to eyesight or lashes when managed properly. But there are specific situations where you should not wait and watch.
- Lash loss that has been ongoing for more than 3 months despite consistent lid hygiene: suggests either inadequate treatment or an underlying issue like Demodex infestation or scarring.
- Noticeably scarred or thickened eyelid margin: a sign of recurrent ulcerative disease that may have caused follicle destruction.
- Trichiasis (lashes turning inward and scratching your eye): this needs clinical management and can cause corneal damage if left untreated.
- Sore or ulcerated areas at the eyelid margin: possible marginal ulcers that need prompt treatment to prevent further follicle damage.
- Any suggestion of a systemic condition: some diseases that mimic or worsen blepharitis, including scarring conjunctivitis and certain autoimmune conditions, need ruling out when presentations are severe or unusual.
- Pain, significant vision changes, or photophobia alongside eyelid symptoms: these need same-day evaluation, not a routine appointment.
An eye doctor can distinguish between non-scarring lash loss (where follicles are sleeping, not dead) and scarring loss through clinical examination and sometimes biopsy. That distinction matters enormously for your prognosis and for choosing the right next step. If there is no scarring, you can be genuinely optimistic about regrowth. If there is scarring in specific areas, treatment shifts toward protecting the remaining follicles and managing the lash line as it is.
The bottom line: most people with blepharitis who treat it consistently will see their lashes recover. The window for protecting follicles is now, while inflammation is still the main driver rather than irreversible scarring. Get the lid hygiene routine in place, talk to your eye doctor if things aren't improving in 6 to 8 weeks, and be patient with the biology. Twelve weeks is not a long time to wait for a full lash line back.
FAQ
If my lashes started falling out with blepharitis, when should I expect them to regrow?
Not always. If the follicles were only pushed into a temporary shedding phase, you may notice regrowth within 6 to 12 weeks after eyelid inflammation calms down. If loss keeps expanding or the lash line looks scarred or irregular, regrowth can stall, which raises concern for scarring or an ongoing trigger that has not been controlled.
Can lashes begin to come back before my blepharitis symptoms are fully gone?
You may see some early “stubbly” regrowth even while symptoms persist, but full thickness and length usually lag behind symptom control. A useful approach is to track both: symptom improvement (less crusting, less irritation) and lash-density change, since persistent lid-margin inflammation delays follicle cycling.
What are common mistakes people make when they think lash loss is only from blepharitis?
Avoid assuming shedding is always blepharitis-related. Trichiasis (lashes growing the wrong way) can cause rubbing sensations and corneal irritation, and it may require specific management to stop lash trauma. Also consider other contributors like Demodex, chronic dry eye, contact irritation from cosmetics, or an underlying skin condition affecting the eyelid margin.
Is it safe to remove lashes that look sparse or misdirected while I’m treating blepharitis?
Yes, shaving or tweezing can worsen the problem because it adds friction at the lash line and can irritate already inflamed lid margins. If you must groom, do it minimally and only after your doctor confirms there is no significant misdirection or ulcerative disease that would benefit from targeted treatment first.
How long is too long to wait to see an improvement in lash regrowth?
If blepharitis is active, delaying care makes it more likely that repeated follicular irritation will lead to scarring in high-risk cases. A practical rule: if symptoms or lash loss are not clearly improving within about 6 to 8 weeks of consistent lid hygiene and treatment, arrange a follow-up to confirm the diagnosis and reassess for scarring risk.
How do I know whether my lash loss is likely temporary versus permanent scarring?
If the loss is patchy, if the lash line has visible white atrophic changes, or if lashes look absent in a focal band that does not regrow by around the 3-month mark, ask your eye doctor whether scarring is possible. Clinical exam, sometimes with biopsy, is the key decision point because treatments differ when scarring is present.
Does blepharoplasty change the timeline for lash regrowth compared with blepharitis alone?
Post-blepharoplasty thinning or shedding can be temporary, but persistent worsening beyond the expected recovery window is a red flag. In particular, progression past about 3 months, visible lash-line scarring, or misdirected lashes rubbing the eye should prompt surgical follow-up rather than waiting for spontaneous recovery.
Can I use bimatoprost for lash regrowth if I still have blepharitis symptoms?
Bimatoprost can help some people with sparse lashes by prolonging the growth phase, but it tends to be most appropriate after blepharitis is stable. Starting it while you have significant lid inflammation can increase irritation, so coordinate timing with your eye doctor, especially if you have active conjunctival redness or ocular surface disease.
Is castor oil safe to try during an active flare of blepharitis?
Castor oil is unlikely to cause direct follicle destruction, but it can irritate if applied to an actively inflamed, weepy lid margin. If you try it, use a small amount, avoid getting it into the eye, stop if burning increases, and prioritize lid hygiene and any prescription targeted therapy for Demodex if that is the cause.
Should I take biotin to regrow lashes after blepharitis?
Biotin helps only when there is a deficiency. If you have no deficiency and no specific medical reason to suspect it, adding biotin is unlikely to change lash recovery. If you do supplement, it is better treated as a general nutrition check rather than a targeted blepharitis or follicle-regrowth strategy.
Citations
Eyelashes cycle through anagen (growth), catagen (transition/club stage), and telogen (resting) before shedding; catagen lasts ~15 days per this review, and after telogen the cycle begins anew with anagen.
https://www.ncbi.nlm.nih.gov/books/NBK537278/
A commonly cited practical estimate for regrowth after a lash is lost is ~6–12 weeks if the follicle is intact (marketing/consumer source; not a clinical guideline).
https://thelashlist.com/guides/how-long-eyelashes-grow-back/
Healthline states it typically takes about ~6 weeks for an eyelash to grow back if cut or burned, assuming there is no damage to the follicle or eyelid.
https://www.healthline.com/health/how-long-does-it-take-for-eyelashes-to-grow-back
Blepharitis can be anterior (toward the front of the eyelid affecting eyelashes) or posterior (affecting meibomian glands); the condition can lead to lash loss and misdirected lashes (trichiasis).
https://www.hopkinsmedicine.org/health/conditions-and-diseases/blepharitis
Meibomian gland dysfunction (posterior blepharitis) is associated with inflammation and poor tear-film quality/dry eye; this is part of the mechanism driving chronic eyelid margin dysfunction affecting lash line status.
https://www.clevelandclinicabudhabi.ae/en/health-library/health-resources/diseases-and-conditions/blepharitis-meibomian-gland-disease
Acute ulcerative blepharitis involves bacterial infection of the eyelid margin at lash-follicle origins, and the lash follicles and meibomian glands are involved.
https://www.merckmanuals.com/professional/eye-disorders/eyelid-and-lacrimal-disorders/blepharitis
Recurrent ulcerative blepharitis can cause eyelid scars and loss or misdirection (trichiasis) of eyelashes—evidence that lash loss can become scarring after severe/recurrent disease.
https://www.merckmanuals.com/professional/eye-disorders/eyelid-and-lacrimal-disorders/blepharitis
Scarring alopecia is hair loss caused by destruction of hair follicles, where inflammation destroys follicle structures and scar tissue (fibrosis) prevents hair regeneration.
https://my.clevelandclinic.org/health/diseases/24582-scarring-alopecia
Cicatricial (scarring) alopecia is characterized by a common final pathway: destruction of the hair follicle unit replaced by fibrous tissue; inflammation is the driver that blocks regeneration.
https://pubmed.ncbi.nlm.nih.gov/22494477/
Chronic blepharitis can cause eyelashes to become misdirected (trichiasis), which is a marker of significant eyelid margin disease and may require procedural/surgical management in severe cases.
https://my.clevelandclinic.org/health/diseases/24542-trichiasis
Madarosis (loss of eyelashes) and trichiasis can occur in blepharitis; the article also notes blepharitis cannot be permanently “fixed” but symptoms can often be managed—implying temporary hair cycling vs permanent damage depends on whether follicles are destroyed.
https://www.hopkinsmedicine.org/health/conditions-and-diseases/blepharitis
In Demodex infestation, chronic blepharitis may include recurrent styes and redness/inflammation/itching; persistent inflammation at the lid margin can contribute to worsening eyelid margin damage over time.
https://www.merckmanuals.com/professional/eye-disorders/eyelid-and-lacrimal-disorders/blepharitis
A retrospective review reports that full-thickness eyelid excision of eyelid margin tissue including lashes “does not usually affect postoperative lash numbers,” suggesting many follicles may survive and lash cycling continues—important for anticipating regrowth after eyelid-margin surgery.
https://eye.hms.harvard.edu/publications/retrospective-review-eyelash-number-patients-who-have-undergone-full-thickness
Upper eyelid blepharoplasty can cause transient postoperative changes in tear film parameters; study notes most values returned to baseline by ~6 months (a proxy for recovery from inflammation/ocular surface irritation that can affect eyelid comfort and lash environment).
https://pmc.ncbi.nlm.nih.gov/articles/PMC12121671/
Post-blepharoplasty instructions include avoiding makeup around incisions for the first 7 days, which reduces mechanical/chemical irritation and contact exposure that can worsen eyelid inflammation (a practical regrowth-delayer risk factor).
https://www.umc.edu/Healthcare/ENT/Patient-Handouts/Adult/PSCSC/Blepharoplasty.html
Cochrane reports that lid hygiene (including warm compresses and lid scrubs) showed some symptomatic relief in both anterior and posterior blepharitis, but there is no strong evidence that any treatment fully cures chronic blepharitis.
https://www.cochrane.org/de/evidence/CD005556_interventions-blepharitis
Guidance summary lists that cleaning the eyelid margin can be done by gentle rubbing of the base of the eyelashes using dilute baby shampoo or eyelid cleaner; it also cites a Preferred Practice Pattern recommending this type of lid-hygiene approach.
https://www.college-optometrists.org/coo/media/media/documents/guidance/using%20evidence%20in%20practice/evidence-base-for-the-effectiveness-of-lid-hygiene-in-the-management-of-blepharitis.pdf
NHS patient information states lid hygiene involves a combination of warm compresses, lid massage, and lid scrubs; it frames this as key to controlling inflammation in blepharitis (including posterior blepharitis/MGD).
https://www.cuh.nhs.uk/patient-information/blepharitis/
A randomized prospective trial evaluated terpinen-4-ol lid scrubs (Cliradex) with Microblepharoexfoliation (BlephEx) for Demodex blepharitis (showing an evidence-based lid-scrub approach beyond basic hygiene).
https://pubmed.ncbi.nlm.nih.gov/31939919/
FDA states XDEMVY (lotilaner ophthalmic solution) was approved based on evidence from two clinical trials of 833 patients with Demodex blepharitis, including criteria like collarettes present on upper eyelid lashes and Demodex density thresholds.
https://www.fda.gov/drugs/drug-approvals-and-databases/drug-trials-snapshots-xdemvy
DailyMed prescribing highlights state XDEMVY is indicated for treatment of Demodex blepharitis and was dosed twice daily in each eye in randomized trials.
https://dailymed.nlm.nih.gov/dailymed/fda/fdaDrugXsl.cfm?setid=ccd9e37c-654e-4e84-8c85-6523457df979&type=display
Bimatoprost ophthalmic solution 0.03% is indicated to treat eyelash hypotrichosis by increasing growth (length, thickness, darkness), and it notes that after discontinuation eyelash growth is expected to return to pre-treatment level.
https://dailymed.nlm.nih.gov/dailymed/fda/fdaDrugXsl.cfm?setid=27bef7e1-750a-4ac1-ab5f-e4c0121ffcbc&type=display
DailyMed lists common adverse reactions (incidence ~3%–4%) including eye pruritus, conjunctival hyperemia, and periocular skin hyperpigmentation.
https://dailymed.nlm.nih.gov/dailymed/fda/fdaDrugXsl.cfm?setid=27bef7e1-750a-4ac1-ab5f-e4c0121ffcbc&type=display
Mayo Clinic warns bimatoprost use with caution in patients with eye disease such as a history of iritis/uveitis (relevant to safety considerations for people who already have active ocular inflammation).
https://www.mayoclinic.org/drugs-supplements/bimatoprost-intraocular-route-ophthalmic-route/description/drg-20062270
A PubMed-indexed randomized trial reports clinical improvements in treated eyes including eyelid margin thickening, telangiectasia, eyelash matting, and madarosis among other Demodex/blepharitis features; improvements in staphylococcal and seborrheic eyelash crusting were also greater vs control.
https://pubmed.ncbi.nlm.nih.gov/32422285/
MedicalNewsToday notes there has been no scientific research specifically on castor oil and eyelash growth in the way it’s marketed, despite anecdotal claims.
https://www.medicalnewstoday.com/articles/325541
A recent systematic review concludes current evidence does not support routine biotin supplementation for alopecia-related hair loss in people without documented deficiency.
https://www.mdpi.com/2673-6179/6/2/17
NIH ODS notes biotin deficiency signs can include scaly red rash and conjunctivitis among other systemic findings; this supports the concept that biotin may only help if deficiency exists (rather than for everyone).
https://ods.od.nih.gov/factsheets/Biotin-HealthProfessional/?uid=716126c3b7d63s16
Mayo Clinic states blepharitis usually doesn’t cause permanent damage to eyesight, but it can cause eyelash loss and misdirection (trichiasis) and can lead to a sore on the cornea from chronic irritation.
https://www.mayoclinic.org/health/blepharitis/DS00633
Johns Hopkins notes blepharitis may be anterior or posterior, and it lists complications including madarosis and trichiasis; it also points to conditions that can underlie or mimic severe eyelid disease (including scarring conjunctivitis as an immunologic condition).
https://www.hopkinsmedicine.org/health/conditions-and-diseases/blepharitis
Merck notes ulcerative blepharitis can progress to marginal ulcers; recurrent ulcerative blepharitis can cause eyelid scars and lash misdirection/loss, which increases the likelihood that lash loss may be permanent if follicles are destroyed.
https://www.merckmanuals.com/professional/eye-disorders/eyelid-and-lacrimal-disorders/blepharitis
Medscape clinical overview emphasizes distinguishing scarring vs nonscarring hair loss—scarring processes involve loss/atrophy of follicular ostia and often (not always) clinical inflammation; histologic confirmation is best for confirming fibrosing/scarring with follicle loss.
https://emedicine.medscape.com/article/1073559-overview
FDA’s trial snapshot shows that Demodex blepharitis severity is assessed using lash “collarette” presence on lashes and eyelid margin erythema plus Demodex density, illustrating how clinicians quantify eyelid disease severity that correlates with lash involvement.
https://www.fda.gov/drugs/drug-approvals-and-databases/drug-trials-snapshots-xdemvy
Will Eyelashes Grow Back After Chemo? Timeline and Tips
Learn if eyelashes regrow after chemo, typical timeline, key factors, and safe at-home tips plus what to avoid.


